Day 5: Live From the ISOO 2019!
Day 5 at the ISOO: Corneal & Conjunctival Cancers
Every two years, eye cancer specialists worldwide convene at the International Society of Ocular Oncology Conference in order to review latest research and encourage international collaboration within the field of ophthalmic oncology.
For details on the ISOO Biennial Conference, read more here.
The final day of the ISOO was dedicated solely to cancers of the conjunctiva, lid, and orbit. Another day filled with research findings and discussion on proper treatment and lesser-known, evidently effective therapeutic techniques.
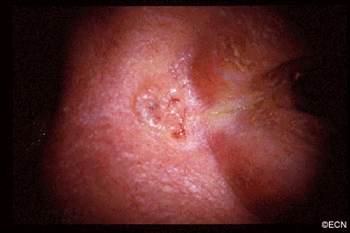
OSSN: Is Surgery Really Necessary?

Is surgery necessary? Dr. Sonal Chaugule asked the question in the paper, Topical chemotherapy for giant ocular surface squamous neoplasia of the conjunctiva and cornea, published alongside Dr. Paul Finger and Dr. Jennifer Park. In the case of ocular surface squamous neoplasia (OSSN), the standard of treatment for years has been surgical excision with adjuvant cryotherapy. However, Chaugule and Finger performed this study in order to compare chemotherapeutic eye drops versus the surgical standard. The eye drops alone have the benefits of convenience and avoidance of complications (however unlikely) from surgery. Ultimately, chemotherapy was found to be sufficient treatment for even giant OSSN. The found that “ topical therapy treated the entire ocular surface and avoided surgical intervention … topical chemotherapy [also] resulted in less scarring and stem cell loss compared to [surgery]. Clearly, larger tumors than widely expected can be controlled with topical chemotherapy alone.”
The full text is available, public-access here.
Palladium Succeeds with Monocular Patient

Our now-graduated fellow Dr. Ekaterina Semenova presented on an already-blogged about, very unique case. A patient had only one functioning eye, and had previously undergone a corneal transplant in this eye. After treating this patient with Palladium-103 plaque brachytherapy through the natural and transplanted cornea, the tumor was found to be controlled and the patient’s vision was conserved.
Read about this case in greater detail on our blog here.
Super-Thick Amniotic Membrane Grafts for Eye Cancer Patients

Another ECF graduate, Dr. Puneet Jain, presented on Super Thick Amniotic Membrane Graft (ST-AMG) Successfully Used for Ocular Surface Reconstruction. Compared to the often-used single-layer amniotic membrane graft, the larger grafts allow for greater patient comfort, as well as greater ease of suture, increased likelihood of remaining in place for the required duration, as well as decreased likelihood of tearing.
Read about this case in greater detail on our blog here.
Keratoacanthoma: An Unusual Location!
A fellow of Dr. Santosh Honavar at The Centre for Sight in Hyderabad, India, Dr. Ankit Singh Tomar will be joining us as the most recent Eye Cancer Foundation fellow. He presented a unique case of a conjunctival keratoacanthoma on the tarsal conjunctiva. It was the first reported case of this extremely unique pathology, and was managed surgically without complications at The Centre for Sight.
We hope to see more great research from Dr. Tomar after he joins us for his fellowship training in ophthalmic oncology her at The New York Eye Cancer Center.

Welcome to our new fellow, Dr. Tomar!
The End, For Now
This marks the final day of the conference and it has since come to a close, though many plans have been made for international cooperation, multi-center databases, and collaborative research so that eye cancer patients worldwide will one day not only have access to care, but have access to the best care we have available. Progress is being made behind the scenes as we speak, and we hope to bring you amazing news for the next conference in 2021.
Until then, thank you for your attention and we thank the amazing physicians and researchers for their great work.


Remember — you can always be a part of our research and international fellowship training by giving a gift to The Eye Cancer Foundation. Dozens of papers this year were presented due to funding from The ECF.