Retinoblastoma
By Paul T. Finger, MD
Description
Retinoblastoma is the most common intraocular cancer of childhood and affects approximately 300 children in the United States each year. More than 96% of children in North America and Europe are cured of retinoblastoma due to early detection and treatment of the affected eye. This is not true for children in countries that do not have eye cancer specialists.
Unfortunately, some children can have both eyes affected. Whenever possible, eye-cancer specialists try to save a child’s eye and preserve their vision.
Symptoms
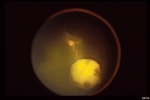
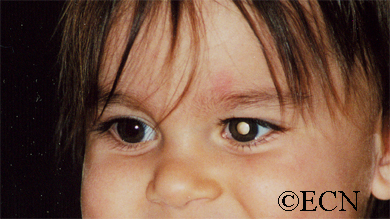
Leukocoria (white pupil) and misaligned eyes (strabismus) are the most common signs of retinoblastoma. In other cases, the child may have developed neovascular glaucoma and may be in pain. Longstanding glaucoma can cause enlargement of the eye (buphthalmos). Children with neovascular glaucoma and enlargement of the eye are at greater risk for extraocular spread of their retinoblastoma.
A family history of retinoblastoma can be very important. Retinoblastoma was the first cancer to be directly associated with a genetic abnormality (Deletions or mutation of the q14 band of chromosome 13). Retinoblastoma can occur sporadically (without a family history) or it can be inherited (with a family history).
If a genetic mutation is found there is a 45-50% chance that the parents will have another child with retinoblastoma. If there is no family history and no mutation is found, the risk of having a second child with retinoblastoma is 2-5%. The average age of children first diagnosed with retinoblastoma is 18 months (typical range 0 to 36 months).
Diagnosis
More than 75% of children with retinoblastoma are first noted to have a “white-pupil” (which the doctors call leukocoria), or poorly aligned eyes (which the doctors call strabismus), or a red and painful eye (usually due to glaucoma). Other eye diseases which can cause these symptoms include congenital cataract, Toxocara canis, Coat’s disease, and persistent hypertrophic primary vitreous (PHPV). These diseases may look like retinoblastoma, but by performing an eye examination under anesthesia (EUA), specialized blood tests, digital photography, radiographic scans, and ultrasound evaluations ophthalmic oncologists can diagnose intraocular retinoblastoma in over 95% of cases. In order to be 100% correct all the time, eye-cancer specialists would have to perform a biopsy. Biopsies of intraocular retinoblastoma are avoided in order to prevent cancer cells from spreading outside of the eye.
The presence of orbital extension, uveal involvement, and optic nerve invasion are known risk factors for the development of metastatic retinoblastoma.
Treatments
Retinoblastoma treatment typically requires the cooperation of an ophthalmic oncologist, pediatric oncologist, and radiation therapist. Over the last 30 years, treatment has evolved from simple enucleation (removal of the eye), to eye-sparing radiotherapy, and more recently to chemotherapy-based multi-modality therapy (for selected cases). Intra-arterial chemotherapy (IAC) has recently been investigated to save eyes, vision and spare the child from systemic chemotherapy.
Though retinoblastoma has been cured by external beam irradiation, investigators have found that radiation may cause an increase in the risk of developing second cancers later in life.
Protocols are currently being evaluated to use chemotherapy to shrink the retinoblastoma in order to treat them with laser therapy, freezing therapy (cryotherapy), and local “plaque” radiation. Where applicable, these techniques are thought to be safer than external beam irradiation for retinoblastoma. Intra-arterial chemotherapy is a newer method of perfusing the eye with chemotherapy, used for selected cases.
Treatment of retinoblastoma often requires a team of doctors made up of ophthalmic, radiation and pediatric oncologists. These doctors should evaluate your child, discuss all the different forms of treatment, and make them available.









