Case #12: PAM With Atypia
By Paul T. Finger, MD
Impression
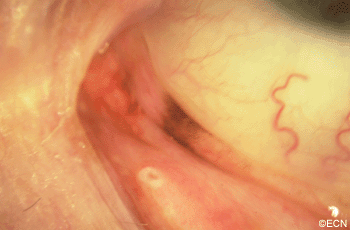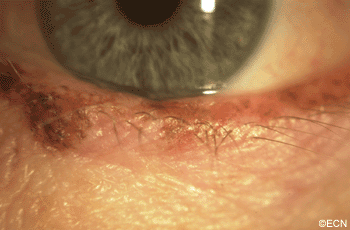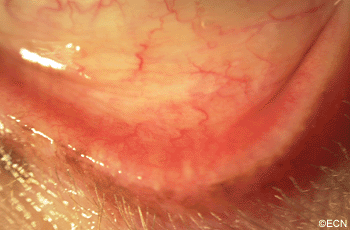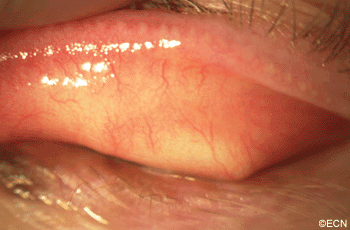
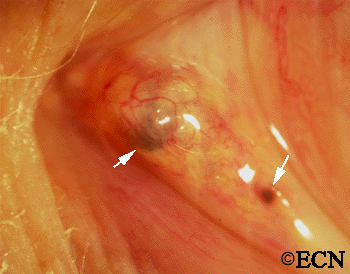
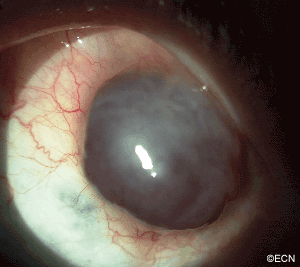
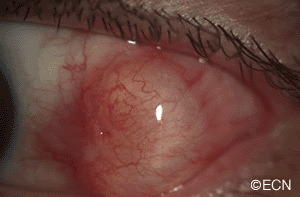
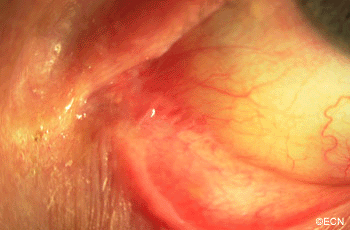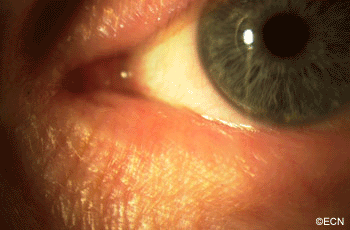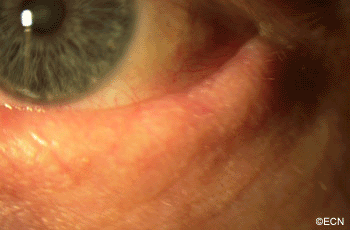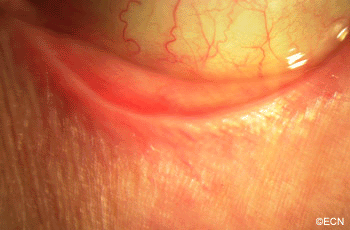
PAM with Atypia with Eyelid Extension.
*Note* This risks and benefits of observation, exenteration, excision with and without cryotherapy and/or topical mitomycin, as well as radiation were discussed with this patient in detail. Primary excision with subsequent topical mitomycin therapy was recommended and performed. The nodular and resectable areas were removed. Topical mitomycin was employed to address the residual diseased epithelium.
Comment
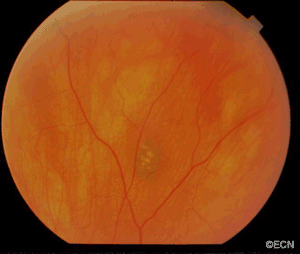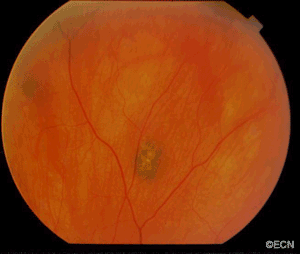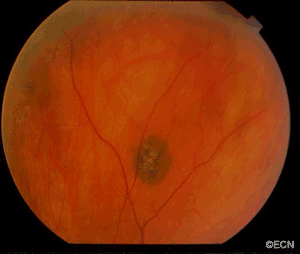
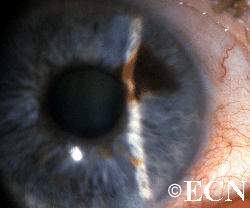
This case presents several classic findings of PAM as well as the unusual finding of extension onto the lower eyelid. Other findings of conjunctival melanomas and primary acquired melanosis include thickness, neovascularization, and corneal epithelial extension. Intraocular extension is very rare, but should this tumor recur, orbital invasion is not uncommon.
Your Questions or Comments
Melanie Kazlas, M.D.
Director of Pediatric Ophthalmology
Boston Medical Center
Question: Yesterday I saw a 10 year old Hispanic/African American child for a routine visit. He had salt and pepper melanosis in the inferior fornix OS>OD as well as a flat pigmented lesion of the nasal inferior tarsal conjunctiva (2x2mm). I often see perilimbal melanosis in my darkly pigmented patients. Can my patient also be classified as having “racial” melanosis?
Answer: I too see a lot of racial melanosis. As a general rule, if it is bilateral, it is probably racial melanosis. As you have noted (unlike your case) racial melanosis primarily involves the bulbar conjunctiva. It is also important to know that nevi can grow during puberty.
In general, I photograph and follow most of these patients. Photography has been made relatively inexpensive and easier by digital technology. My threshold for biopsy of suspicious or growing lesions is low. Make sure an ophthalmic pathologist sees the specimen.

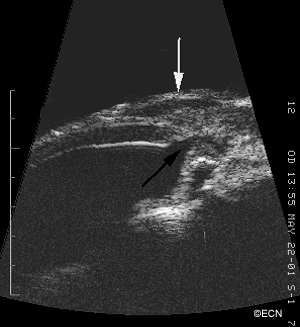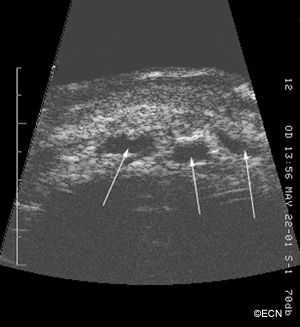
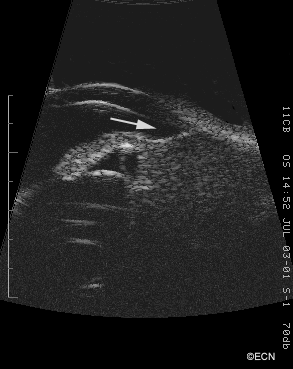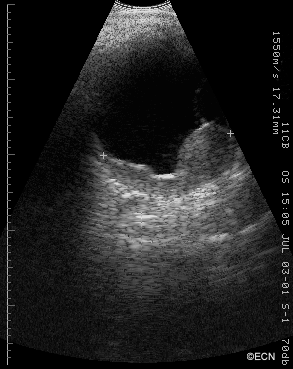
![[10 MHz] 3D Ultrasonography Reveals - *Note* Ultrasonography reveals an open funnel retinal detachment (white arrow). Note the echolucent vitreous humor. The posterior choroidal detachments (black arrows) exhibit variable internal reflectivity consistent with blood. A = anterior, S = superior, T = temporal.](https://eyecancer.com/wp-content/uploads/2016/05/case111.gif)
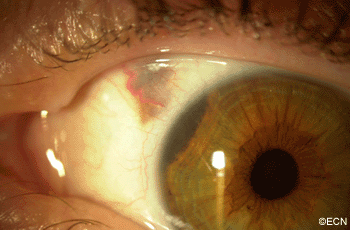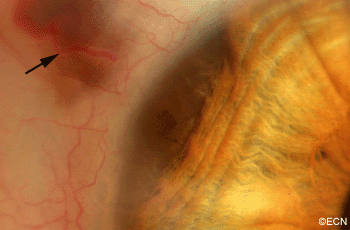
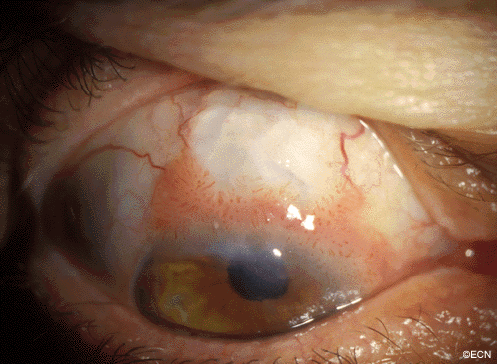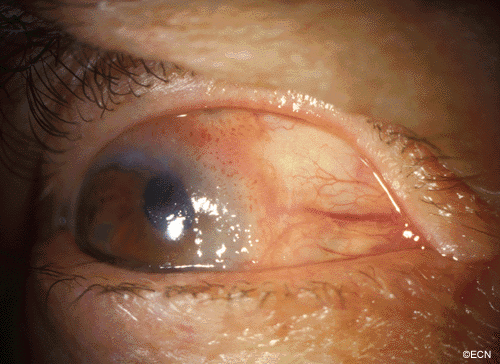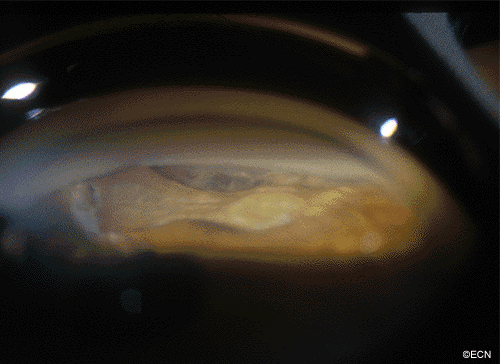 A man with a past ocular history of glaucoma (status-post trabeculectomy) and macular degeneration was referred to The New York Eye Cancer Center with squamous conjunctival neoplasia affecting his right eye.
A man with a past ocular history of glaucoma (status-post trabeculectomy) and macular degeneration was referred to The New York Eye Cancer Center with squamous conjunctival neoplasia affecting his right eye.