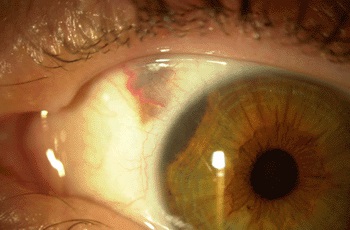
A doctor who recently completed fellowship training supported by The Eye Cancer Foundation (ECF) is providing eye cancer treatment in an area of India currently lacking any trained specialists in ocular oncology.
Dr. Bikramjit Pal worked under Dr. Tero Kivelä at the Helsinki University Eye Hospital during his six-month fellowship from October 2015 through March 2016. In addition to mentoring from Dr. Kivelä, Dr. Pal learned from a wide range of highly trained medical professionals at the hospital. He actively participated in daily patient workups in the Ocular Oncology Service and observed and assisted in the treatment of eye cancer patients.
During his training, Dr. Pal was exposed to a wide range of procedures and treatments, including outpatient and intraoperative transpupillary thermotherapy, ruthenium and iodine plaque brachytherapy, conjunctival surgery, and intravitreal chemotherapy. He was involved in the treatment of conjunctival carcinoma, conjunctival melanoma, ocular adnexal and intraocular lymphoma, uveal melanoma, and retinoblastoma. He also had the opportunity to participate in one-on-one teaching in the latest diagnostic techniques related to eye cancer under the supervision of senior consultants.
In addition to his practical training, Dr. Pal also participated in research studies during his fellowship. He took part in an ocular oncology journal club and undertook three scientific projects, including one case report and two observational case series. Dr. Kivelä praised Dr. Pals work during his fellowship training:
“Dr Pal has shown keen interest in his studies, an excellent working knowledge of fundamentals of ophthalmology, and he has been a most avid observer.”
The Eye Cancer Foundation offers fellowships to doctors from unserved and underserved countries, providing specialized training in the treatment of retinoblastoma and other eye cancers. Once they complete their training, ECF fellows commit to return home to create eye cancer treatment programs.
Dr. Pal plans to begin oncology services at a tertiary eye care facility in Kolkata. This center serves a huge population, not only in eastern India, but also in the neighboring countries of Nepal and Bangladesh. Dr. Pal said he was eager to apply his training in his home country.
“In India, we deal with retinoblastoma so often; hence my aim is to start with a fully equipped clinic which will provide services to patients having intraocular tumors.”
With Dr. Kivelä’s ECF-sponsored fellowship training, Dr. Pal will be able to provide high-quality care to eye cancer patients who would otherwise have little to no access to treatment. This translates to saved vision and lives. Dr. Kivelä will continue to mentor Dr. Pal, providing long-distance consultative support and will soon visit Dr. Pal’s center.
Through the recently launched 2020 Campaign, The Eye Cancer Foundation plans to multiply this success story across the world. With your help, we can train 20 eye cancer specialists to work in 20 countries by 2020.
Our immediate goal with the 2020 Campaign is to save the lives of 1,000 children by 2020. But that’s only the beginning. Our ability to train doctors and supply them with the equipment they need to properly diagnose and treat retinoblastoma is only limited by the generosity of our donors.
You can become part of the cure with a one-time or recurring donation to The Eye Cancer Foundation. Click HERE to donate today.
For more information on The Eye Cancer Foundation Fellowships, including how to apply, click HERE.






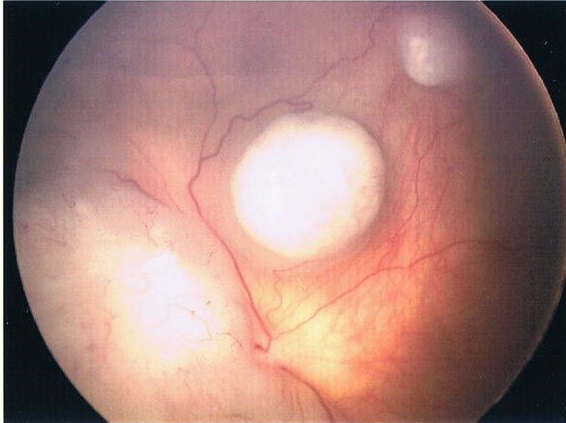


 who were diagnosed at different stages in the disease. This allowed him to observe a wide variety of treatment regimens, including systemic chemotherapy, intraocular chemotherapy, intra-arterial systemic chemotherapy, focal consolidation therapies (e.g. laser and “freezing” cryotherapy), radioactive plaque therapy, external beam radiation therapy, and when necessary – removal of cancer-filled eyes.
who were diagnosed at different stages in the disease. This allowed him to observe a wide variety of treatment regimens, including systemic chemotherapy, intraocular chemotherapy, intra-arterial systemic chemotherapy, focal consolidation therapies (e.g. laser and “freezing” cryotherapy), radioactive plaque therapy, external beam radiation therapy, and when necessary – removal of cancer-filled eyes.