Think of Sunglasses As Sunblock For Your Eyes
“Think of sunglasses as sunblock for your eyes,” is an oft-repeated slogan around the New York Eye Cancer Center. While most people tend to think of sunglasses as just a fashion statement, they may actually be a key defense against eye cancer. Sun causes damage to eye tissues just like it does to skin – but since you can’t put sunblock on your eyeballs, you should make sure to wear UV-cancelling sunglasses as well.

Fortunately, other groups are joining in this educational effort.
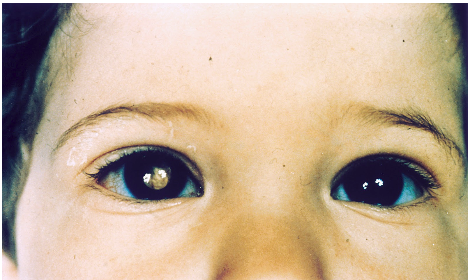
Last month, Vision Express Stores in Great Britain gave away sunglasses to mark World Retinoblastoma Awareness Week. We applaud this initiative and would encourage similar efforts here in North America.
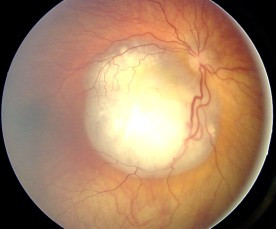
Ocular melanoma is the most common primary eye tumor in adults. There are around 2,000 new cases every year. These tumors are closely related to skin cancer. Since exposure to the sun is a known risk factor for skin cancer, it follows that UV rays from the sun may also increase the risk of developing this form of eye cancer. There is circumstantial evidence linking exposure to sunlight and ocular melanoma. This form of eye cancer is more common in patients with blue eyes, and who work in outdoor occupations.
When any form of light is absorbed by the body, a reaction occurs resulting in heat and chemical changes. Ultraviolet light rays are particularly energetic and cause more chemical reactions in ocular tissues than visible light. This means more potential damage to the eye.
While the link between sunlight and eye melanomas is not conclusively proven, it is worth a small precaution that will make you look like James Dean anyway!
A good pair of sunglasses will block all UVA, UVB, and UVC rays. You want to make sure the glasses provide 100% UV protection. Many optical shop have a machine called a photometer that measures UV transmission through glasses. You want to wear sunglasses that block all UV radiation or light under 400 nm in wavelength.
Buyer beware: Shades that don’t offer this protection – or cheap pairs that fraudulently claim to – may actually increase the risk of eye cancer by allowing more UV light into the eye.
So choose wisely, make that fashion statement, and protect your eyes at the same time.