By Paul T. Finger, MD
Description
Adenocarcinomas and adenomas typically arise from a part of the retina called the retinal pigment epithelium or RPE. They can also occur in the ciliary body. Though all are rare, benign adenomas are much more common than RPE cancers. Less than 20 malignant adenocarcinomas of the RPE have ever been reported.
Further, during the modern era of reporting, malignant adenocarcinomas of the RPE have never been reported to spread to other parts of the body.
In the past, almost all RPE adenocarcinomas were clinically diagnosed as atypical choroidal melanomas and the eyes were enucleated. In Dr. Finger’s review of the literature, RPE adenocarcinomas were found to be more common in females, more likely to cause intraocular inflammation (atypical for choroidal melanomas) and have responded poorly to radiation therapy.
Symptoms
Patients with adenomas of the retinal pigment epithelium typically have no symptoms. These tumors are found during routine eye examination and referred to eye tumor specialists for further evaluation.
Diagnosis
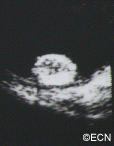
Retinal adenoma and adenocarcinoma will appear black. They originate from the retina, so they are not likely to have a surrounding or overlying retinal detachment. Adenomas appear dark. “block fluorescence” on fluorescein angiography.
Ultrasound may be helpful in distinguishing adenoma and adenocarcinoma of the RPE from uveal melanomas. Consider that they tend to arise from the retina above Bruch’s membrane. Therefore, they appear to be stuck on rather than growing from the underlying choroid. Several investigators have noted a tuberous rather than collar-button or dome-shape.
Treatments
Retinal adenoma should be photographed, measured by ultrasound and followed for evidence of growth prior to consideration of treatment.
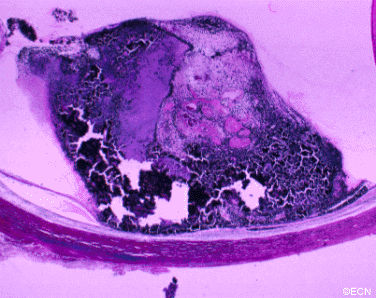
In the rare instance of retinal adenocarcinoma, most patients have been enucleated with a presumed diagnosis of choroidal melanoma. Should adenocarcinoma of the retinal pigment epithelium be suspected, a biopsy should be considered. Characteristics of RPE adenocarcinoma are a female patient with a dark intraocular tumor and associated with iritis and/or uveitis.









