 The methods for diagnosis of patients with iris, iridociliary and anterior uveal tumors have changed in recent years.
The methods for diagnosis of patients with iris, iridociliary and anterior uveal tumors have changed in recent years.
Traditionally, patients diagnosed with an iris or iridociliary melanoma have undergone intraocular surgery to “cut out” the tumor. But today, Dr. Finger rarely has to remove the tumor, instead opting for destroying it with an external application of plaque radiation therapy.
It is well known that intraocular surgeries carry greater risk of intraocular infection, hemorrhage, retinal detachment and cataract. In addition, removal of the iris (whose function is to limit the amount of light entering the eye) typically results in a large “key-hole” pupil and symptoms of glare. Over the last 20 years, Dr. Finger has found that plaque radiation therapy destroys the tumor and usually preserves iris function, thus making his patients happier with their results.
Eye cancer specialists used to worry about radiation retinopathy or corneal opacity after plaque radiation for iris melanoma. However, with over 20 years of experience with palladium-103 plaque therapy, it appears that only cataract is the primary complication. These lens opacities are easily repaired with standard cataract surgery. The risk of radiation retinopathy and optic neuropathy is minimal.
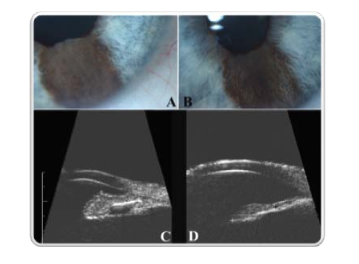
The advent of high-frequency ultrasound imaging has revolutionized the diagnosis of cancers affecting the iris.
For more information on the diagnosis and treatment iris and ciliary body melanoma, and Dr. Finger’s research in the area download the PDF:









