A paper co-authored by Dr. Bikramjit P. Pal highlights a study conducted under the guidance of Dr. Tero Kivelä while supported by a fellowship grant provided by The Eye Cancer Foundation.
Dr. Pal worked under Dr. Kivelä at the Helsinki University Eye Hospital during a six-month fellowship from October 2015 through March 2016. During the fellowship, they conducted a study to follow the course of blood–brain barrier disruption maculopathy in a patient undergoing treatment for relapsed central nervous system lymphoma.
 A primary central nervous system (CNS) lymphoma is a cancer inside the skull. Thankfully rare, CNS lymphomas account for about 3% of central nervous system cancers. Chemotherapy treatment is difficult due to the blood-brain barrier, a highly selective semipermeable membrane that separates circulating blood from the brain. Because many substances can’t pass through it, the blood-brain barrier protects the brain from most pathogens, but also limits the effectiveness of many chemotherapy agents.
A primary central nervous system (CNS) lymphoma is a cancer inside the skull. Thankfully rare, CNS lymphomas account for about 3% of central nervous system cancers. Chemotherapy treatment is difficult due to the blood-brain barrier, a highly selective semipermeable membrane that separates circulating blood from the brain. Because many substances can’t pass through it, the blood-brain barrier protects the brain from most pathogens, but also limits the effectiveness of many chemotherapy agents.
A process called blood-brain barrier disruption (BBBD) can improve chemotherapy effectiveness in patients suffering from central nervous system lymphoma. The process involves the infusion of a warm hyperosmotic agent that allows the chemotherapy drugs to cross the barrier. BBBD results in a higher concentration of the drug by a factor of 50 to 100 times as compared with the standard intravenous route.
But there are risks involved in this BBBD-aided mode of treatment. Because the eye is part of the CNS and also shielded by the blood brain barrier, BBBD can cause a complication known as maculopathy. Maculopathy is damage to the macula (the functional center of the retina) resulting in a progressive loss of central vision. Mild to moderate loss of visual acuity (VA), and a nonprogressive nature, are the hallmarks of this condition in patients undergoing BBBD.
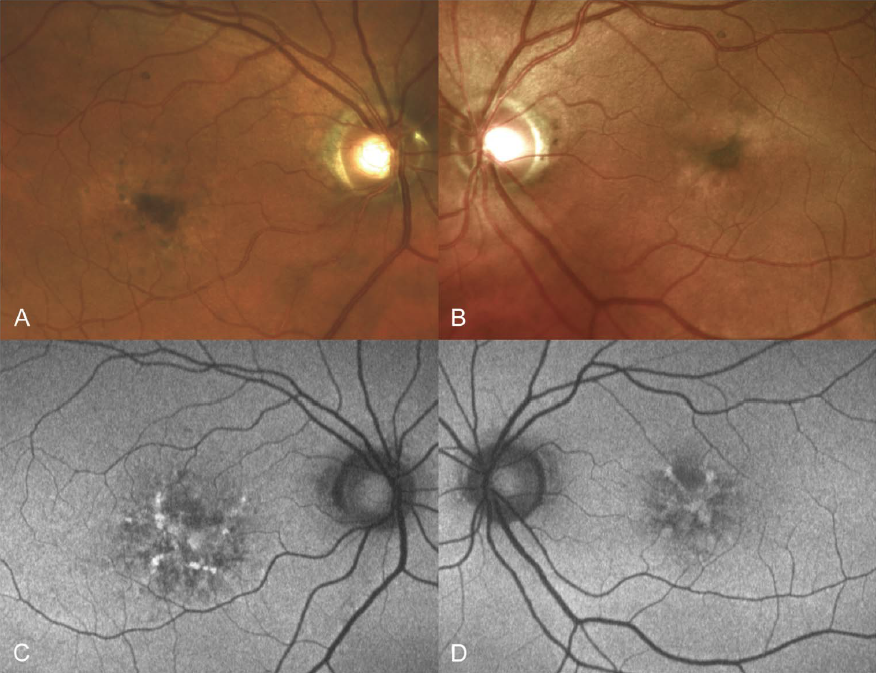
The study followed a 57-year-old patient diagnosed with central nervous system large B-cell lymphoma. He had a normal ophthalmic evaluation on his first visit. He was treated with blood–brain barrier disruption therapy and intra-arterial methotrexate. During the course of the therapy, he developed maculopathy with minimal eventual loss of visual acuity to 20/32 and 20/25 in his right and left eye respectively.
The study helped track the progression of maculopathy and provides some insight into the processes involved. It will certainly pave the way for further study.
“Although the maculopathy seems to be non-progressive and non-vision threatening, and the BBBD therapy usually is life saving as it was for our patient and cannot be abandoned, patients need regular follow-up as the full spectrum of this condition is probably not yet completely understood. Future studies incorporating fundus autofluorescence and OCT angiography may help in this regard.”

Dr. Pal acknowledged the support of The Eye Cancer Foundation fellowship grant in the paper.
The ECF offers fellowships to doctors from unserved and underserved countries, providing specialized training in the treatment of retinoblastoma and other eye cancers. Once they complete their training, ECF fellows commit to return home to create eye cancer treatment programs.
Dr. Pal plans to begin oncology services at a tertiary eye care facility in Kolkata. This center serves a huge population, not only in eastern India, but also in the neighboring countries of Nepal and Bangladesh.
Through its 2020 Campaign, The Eye Cancer Foundation plans to multiply this success story across the world. With your help, we can train 20 eye cancer specialists to work in 20 countries by 2020.
Our immediate 2020 Campaign goal is to save the lives of 1,000 children by 2020. But that’s only the beginning. Our ability to train doctors and supply them with the equipment they need to properly diagnose and treat retinoblastoma is only limited by the generosity of our donors.
You can become part of the cure with a one-time or recurring donation to The Eye Cancer Foundation. Click HERE to donate today.









