Doesn’t every patient want to know
the past results of the doctor they select for their treatment?
In response to this need, The New York Eye Cancer Center is the first eye cancer practice to report its results on the world-wide-web.
Now these results are available to everyone.
Choose your cancer below to view results:
About this Data:
– Data includes only patients treated by Dr. Finger at The New York Eye Cancer Center.
– Patient data is confidential, anonymous, and HIPAA-compliant.
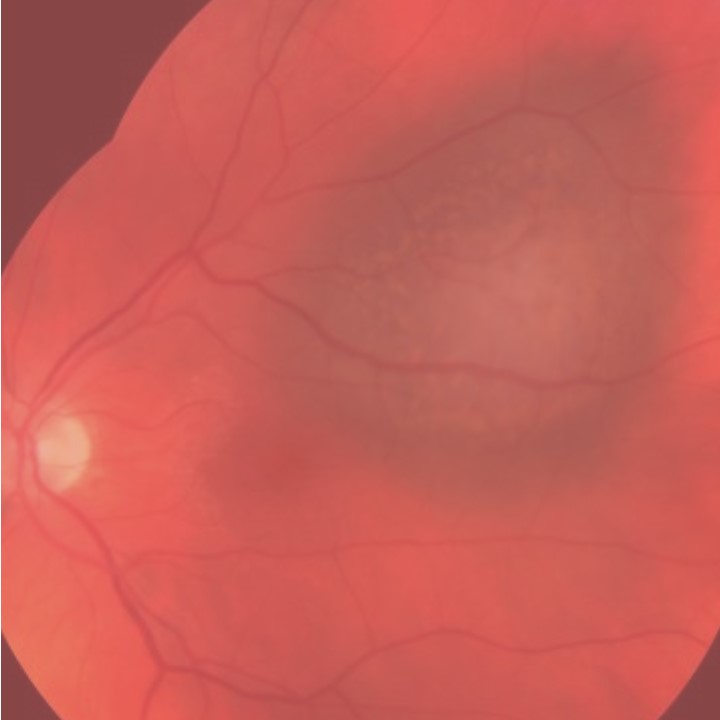
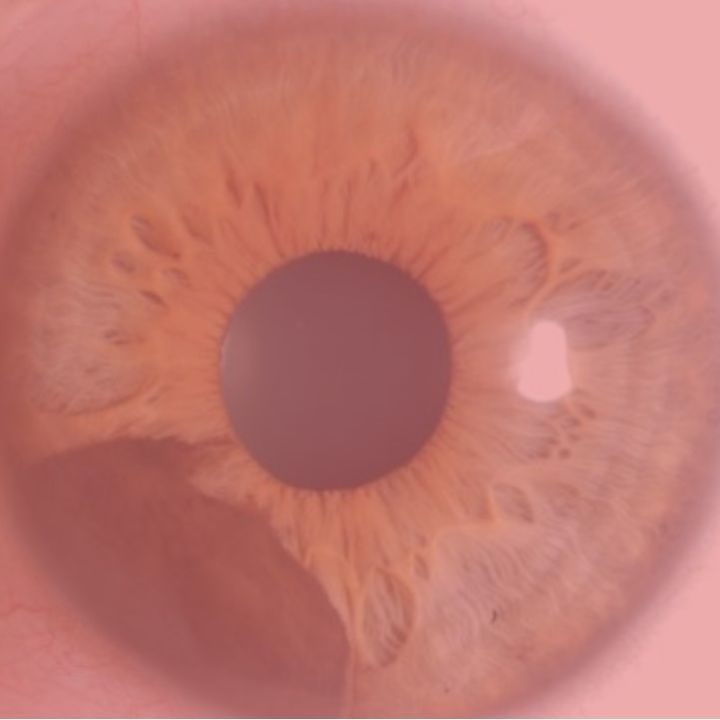
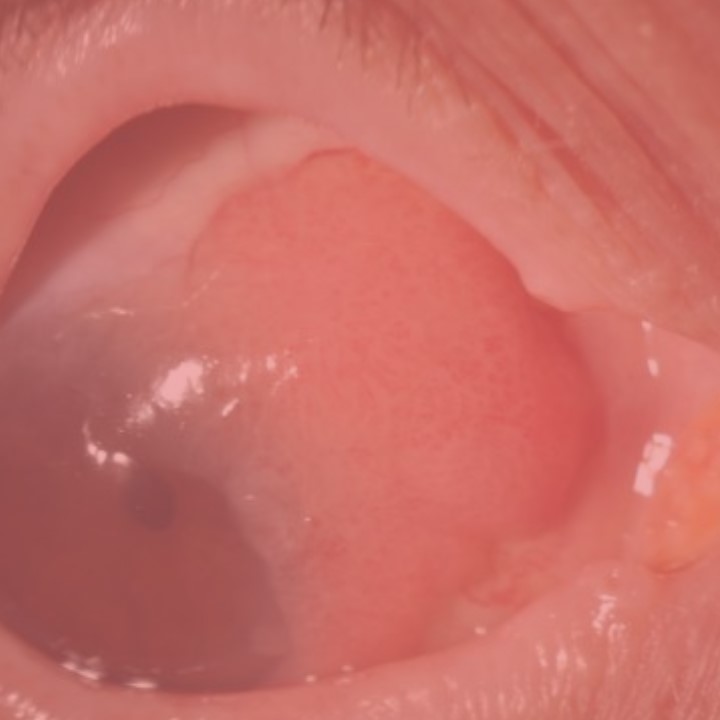
– Starting from December 2017, every patient’s outcome with these select diseases (choroidal melanoma, iris ciliary body melanoma,
and squamous conjunctival malignancy) was anonymously recorded at each visit to The New York Eye Cancer Center. There is no selection bias.
– Only patients who return for regular follow-ups are included; no patient who has been more than 12 months lost to follow-up is included.
– Enucleated patients are not included in the visual acuity outcome.
– The percentage of patients who had to, or preferred to have their eye removed (enucleation) as initial (primary) treatment.
– Visual acuity of hand motion, light perception, or no light perception are given a value of “0” and are therefore not averaged into the system.