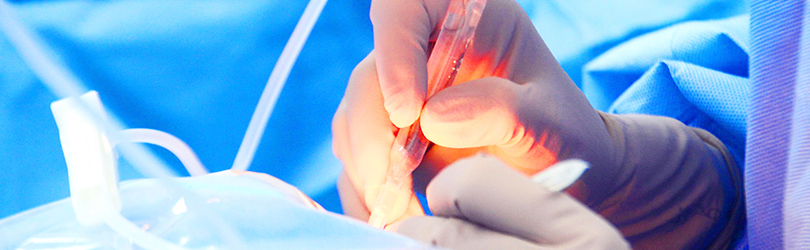
Radiation Plaque Therapy
In 1991, Dr. Finger discovered that palladium-103 radiation typically offered a better radiation distribution (within the eye) that the more widely used iodine-125 radiation in ophthalmic plaques. Over the following 28 years, Dr. Finger has periodically published his experience with palladium-103 plaque therapy to treat intraocular melanoma. He has among the highest local tumor control, eye, and visual acuity retention rates when compared to other published studies/clinical centers. Vision retention means keeping your vision. These outcomes are related to careful treatment planning, selection of the best radiation source and a surgeon who has been carefully treating patients with ophthalmic radiation therapy.
Finger-Tip Cryotherapy Applicators

Dr. Finger introduced the “Finger-tip” cryotherapy “freezing” applicators for treatment of malignant conjunctival and corneal tumors. Freezing is used to destroy tumors that cannot be removed from the body. Unlike standard cryotherapy probes, Dr. Fingers’ devices are spatulated (flat oval surfaces). Thus they offer larger and more uniform targeted zones compared to retinal cryotherapy tips often used in other centers. Simply put, using these probes decreases the chance of missing a small area of tumor. Dr. Finger has also used these large cryotherapy probes to grasp tumors of the orbit and facilitate enucleation surgery.
The Finger Iridectomy Technique
Dr. Finger was unhappy about the safety of needle biopsy. He didn’t like the fact that the biopsy needles were pointed and sharp along their edges (see image below). So Dr. Finger invented the Finger Iridectomy Technique.
Dr. Finger says,
“Think about the relative safety of having a needle with sharp edges and a pointy tip inside the anterior chamber of the eye. Then compare that to the rounded, relatively safe aspiration cutter tip (below). Then consider that once the needle is in the eye, the surgeon must poke, cut and scrape the tumor with the sharp edges to aspirate the freed tissue into the needle hole. Suction into the hole is created by the surgical assistant pulling on a syringe on the other end of extension tubing. This can flatten the anterior chamber with the sharp needle inside. If blood clouds the chamber during biopsy, the surgeon either has a poor or no view and the needle is a poor instrument to aspirate out that blood.”

25-Gauge Tip
——————————————————————————-

25-Gauge Aspiration Cutter Tip: FIT Procedure
Then Dr. Finger says about The Finger Iridectomy Technique:
“In contrast think about the relative safety of placing the rounded aspiration cutter into eye filled with surgical visco-elastic. There are no sharp edges should the patient move. The visco-elastic is thicker than the aqueous water and maintains the depth of the anterior eye chamber during biopsy. The surgeon must only place the portal of the cutter over the tissue to be biopsied. Unlike the needle, the suction is machine limited and controlled by the surgeon using a foot-pedal (like an accelerator on a car). UNLIKE the needle biopsy, there is no poking or scraping of tissue. The relatively controlled FIT aspiration cutting not only retrieves cells for cytology but typically retrieves chunks of tumor so that the pathologist can see the architecture that helps diagnosis”.
This allows Dr. Finger’s pathologists to evaluate cytology, histopathology, and perform immunohistochemical analysis. Thus far FIT biopsy at The New York Eye Cancer Center has been very safe. Dr. Finger has found that this technique almost always (>99%) will get enough tumor to make the diagnosis.
Finger’s Slotted Plaques for Choroidal Melanoma: Near, Touching, Surrounding or Covering the Optic Nerve
Dr. Finger has expanded prior limits to save eyes, vision and life using eye plaque radiation therapy. For example, in the past many patients with intraocular melanoma were advised to have their eye removed if it was too close, touching, surrounding or covering the intraocular optic nerve. However, based on his research measuring the thickness of the optic nerve (as it exits the back of the eye), Dr. Finger invented these special radiation eye plaque able to “cover” the entire tumor and thus allow normal rates of local control (tumor destruction) . This eye and vision-sparing alternative had an 8-mm wide slot that allowed the nerve into the radiation plaque and also allowed the radiation zone to advance beyond the posterior extent of the tumor.. He calls these specially designed devices “Finger’s Slotted Plaques.”
Dr. Finger designed these new radiation devices to work around incorporating the orbital portion of the optic nerve within the plaque. For the first time, the radiation treatment zone (for tumors near and around the optic nerve) was “normalized” and extended to cover the entire tumor. This innovation has improved local control, and saved vision and lives for patients with this previously hard-to-treat choroidal melanoma. See superimposed plaque on a photograph of a melanoma touching and starting to surround the melanoma.
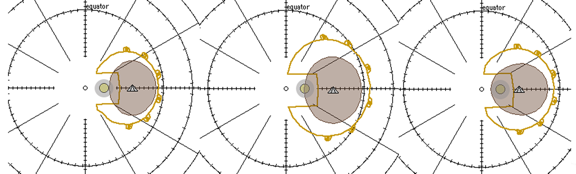
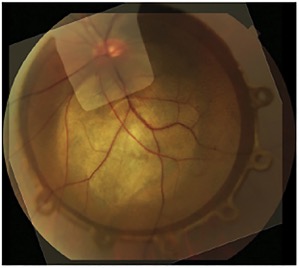
A photograph of a choroidal melanoma touching the optic nerve superimposed on a Fingers’ Slotted Plaque
With Dr. Finger’s slotted plaque innovation and extra-large 24 mm diameter plaques, 94% of patients with choroidal melanoma who are treated at The New York Eye Cancer Center don’t have to have their eye removed (enucleation). This is important because most patients want to keep their eye.
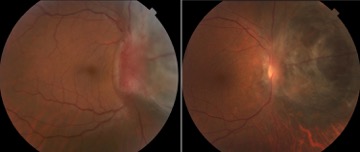
Before and after treatment with Finger’s Slotted Plaques. Notice that the optic nerve head is uncovered as the tumor shrinks away.









